Wellness Testing - Why does my vet keep recommending it?
At some point or another the chances are that your veterinarian has recommended running "wellness" bloodwork on your pet during a visit. While many people appreciate the benefit of wellness testing, there is still some confusion as to what it is and why we (as veterinarians) recommend it. Quite often, the question we're asked is "why run bloodwork, he's acting completely normally"? To fully appreciate why we recommend additional bloodwork on seemingly "normal" pets it's important to understand the thinking behind these recommendations. Many veterinarians (myself included) strive to practice preventive medicine. Preventive medicine is the approach that it's better to prevent a problem in our patients, than react to and treat an already existing (and often more serious) problem down the road. In order to take this proactive approach, we're often looking for signs of impending disease which can sometimes be subtle or require monitoring for change over time. It makes sense that preventing problems is better than trying to play "catch-up" once a disease is in full swing. This isn't to say that all diseases can be addressed this way, but it's good practice to try to prevent illness when we can. Sometimes we can identify potential future problems during our physical examinations - a good example of this would be the prevention of dental disease while examining the mouth. However, the physical exam is just one of the tools we use to assess overall health and sometimes additional testing is needed to identify potential problems. This is especially important because our patients cannot talk to us and tell us how they're feeling. Wellness bloodwork is an example of a tool we use to assess overall health and consists of a comprehensive screen for many diseases. Wellness bloodwork generally consists of a CBC and Biochemical Profile:
CBC: evaluation of red and white blood cells - looks for signs of anemia, clotting disorders and infection (to name a few)
Biochemical Profile: evaluation of body organs such as liver, kidneys, pancreas. Is also used to screen for diseases such as Diabetes Mellitus, Cushings Disease, Thyroid Disease and others.
Recently I was involved in a case that perfectly illustrates how helpful wellness blood testing can be in identifying a potential problem, and initiating therapy in a dog that was showing no signs of disease at all:
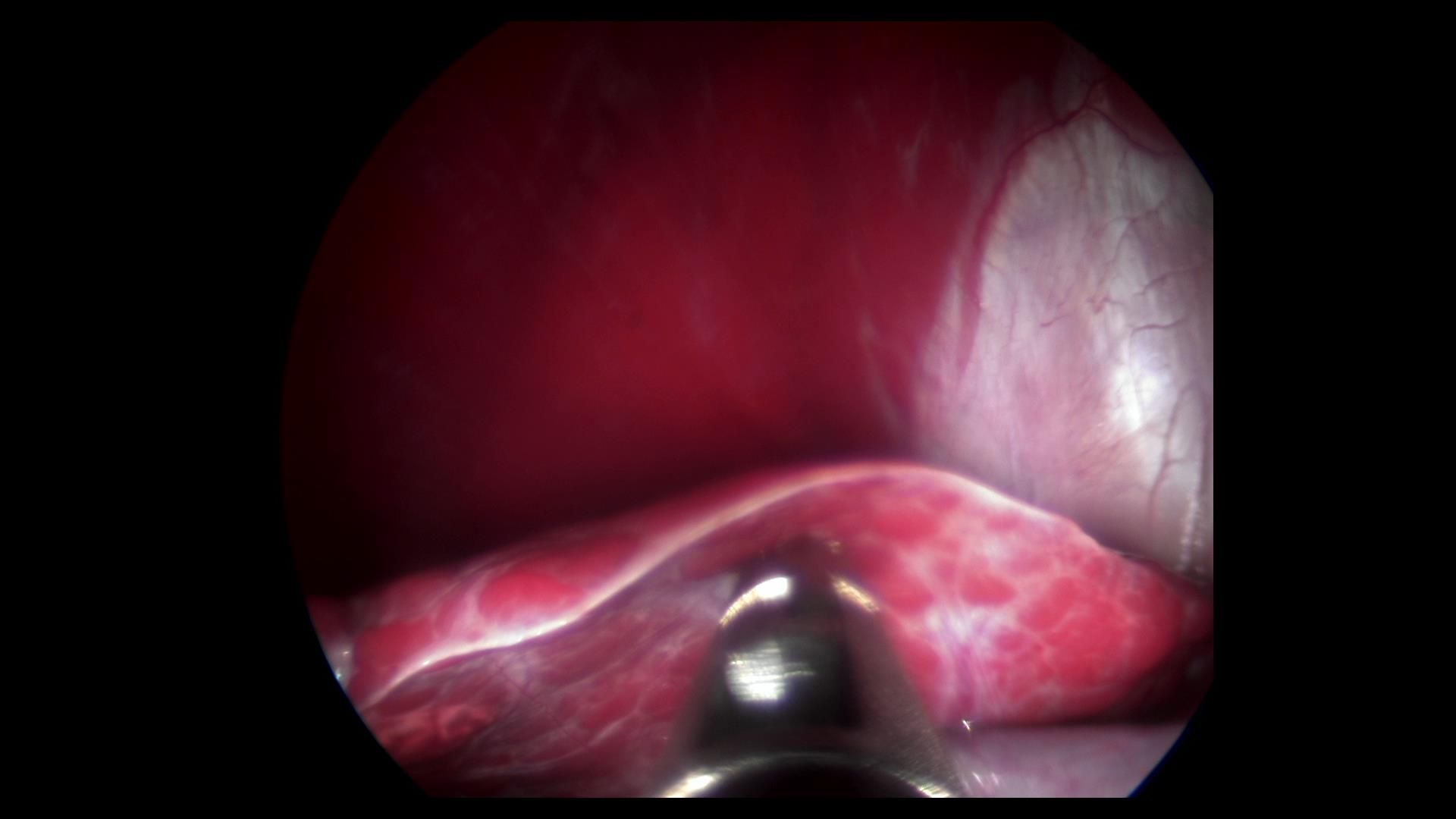
A colleague recently called me in to perform laparoscopic liver biopsies on a 7 year old male neutered Standard Poodle. 2 months prior his owner had brought him in for a general annual exam and wellness bloodwork was performed during this appointment. Clinically the dog was acting completely normal and the owner had no health concerns at all, however the bloodwork came back showing some mild to moderately elevated liver values on the biochemical profile. This can sometimes be a normal fluctuation or minor recent liver insult, so the veterinarian recommended monitoring him at home and rechecking the liver values in about 4-6 weeks time. At the recheck examination, the dog was still behaving normally but the liver values had continued to increase so the decision was made to investigate further with laparoscopic liver biopsies. On laparoscopy, the liver appeared smaller than normal, quite nodular, and there were signs of fibrosis (or scarring). Multiple biopsy samples were taken and sent to the lab for interpretation, with concerns about hepatitis or cancer being the underlying cause.
Luckily, the results confirmed that cancer was not present, but did report generalized nodular growth and scarring throughout (suggestive of a slow chronic disease process but not specific).
While this particular disease may not be 100% curable, specific treatments were started to slow down the progression of disease. By catching something early, this veterinarian will now be able to offer therapies that will provide a higher quality of life for a longer period of time. By contrast, if this problem had been identified later due to the dog becoming clinically ill there would have been very little that could have been done to help him (i.e. the damage is already done and he is suffering from liver failure).
Remember: Wellness bloodwork often allows us to identify issues early and prevent smaller problems from becoming big ones!
Recent Posts